
Recently I had the privilege of attending The Pacific Community (SPC) 14th annual Pacific Heads of Health (PHoH) meeting in Nadi, Fiji. The annual meeting, established in 1995, has as its main goal addressing the health of people living throughout the Pacific Islands. SPC in conjunction with the World Health Organization (WHO) and the Pacific Island Health Officers Association (PIHOA) co-chaired the meeting that brought together the Permanent Secretaries of Health from each Pacific Island Country, as well as partner agencies. A number of salient regional health topics were reviewed and discussed. I was honored to be invited to present for the discussion Vulnerability of Pacific Island Country Hospitals.
While most policy people are familiar with the Pacific Island Forum (PIF), the region’s premier political and economic policy organization, few know about SPC, one of the oldest organizations in the Pacific Region.
SPC was founded in 1947 by Australia, New Zealand, the Netherlands, Great Britain and the United States. Known originally as the South Pacific Commission the organization provided advice to member states on economic, social and health matters impacting the South Pacific Island territories the members oversaw. In 1951 the South Pacific Commission became known as the Secretariate of the Pacific Community (SPC) after the northern Pacific Island US trust territories became members. With individual Pacific Island Countries gaining independence SPC was transformed into an agency offering technical advice, assistance, training, and research to address economic, biological, medical, educational, and social problems. Currently there are 27 member states, each with equal voting rights and there are a number of partners who provide financial as well as technical support. The majority of funding for SPC comes from Australia, New Zealand, the European Union, France and the United States. SPC’s main headquarter is in Noumea, New Caledonia and there are regional offices in Suva Fiji, Port Vila Vanuatu, Honiara Solomon Islands, Pohnpei FSM, and Paris France.
The SPC’s mission is “to progress all Pacific peoples’ rights and well-being through science and knowledge, guided by our deep understanding of Blue Pacific contexts and cultures.” Their divisions currently address a wide range of issues including climate change and environmental sustainability, fisheries, education, human rights, land resources, geoscience, and public health. SPC’s Pacific Data Hub is also a repository for development data and statistics from the Pacific Island region.
The annual Pacific Heads of Health meeting, which falls under the Public Health division of SPC, focuses on reviewing health related topic that are germane to the region through sponsored presentations on topics to consider, reviewing data on current programs and holding discussions on key health issues in order to make recommendations to the Pacific Health Ministers Meeting. The PHoH meeting for all intents and purposes is where much of the Pacific Regions health policy begins. It is an invaluable resource for development partners to become informed about issues that are pertinent to Pacific Island health. This year partner agencies in attendance included US representatives from the US Department of Health and Human Services, the CDC, USAID and the US Embassy in Fiji.
Over the course of the 3 day meeting a large number of health topics were discussed. Some of the key topics that were discussed included:
- Health Information Systems and the role of Digital Health in the Pacific Islands
- Strengthening Health System Resilience to climate mediated impacts
- Healthcare work force
- Tackling Non Communicable Diseases, obesity in children, rising Sexually Transmitted Disease rates and refocusing on TB, malaria and HIV
- Gender based violence and an update on nursing and midwifery programs
Two topics discussed deserve mentioning as development partners should consider addressing them in order to sustainably strengthen Pacific Islands health: PIC healthcare workforce and the PIC vulnerable health systems including infrastructure.
On healthcare workforce: Fiji National University (FNU) shared statistics on the number of students in healthcare tracts for 2019 and 2023 as well as student attrition rates across PICs. Overall post graduate health education enrollment at FNU is down. FNU along with the University of Papua New Guinea School of Medicine and Health Sciences provide the majority of health education for the region. If attrition and decreased enrollment trends persist, maintaining an adequate health workforce could become quite challenging. This is not a new problem. In 2006 Kiribati and Solomon Islands sent 33 and 104 students, respectively, to Escuela Latinoamericana de Medicina (ELAM, the Latin American School of Medicine) in Cuba. While doctor to patient ratios in Kiribati improved from 2.0/10,000 to 6.0/10,000 the large number of students sent to Cuba by Solomon Islands did not significantly improved its doctor patient ratio of 2.4/10,000. This suggests there may be a workforce retention problem. The WHO recommends a ratio of at least 10/10,000. In the US there are 28.2 doctors per 10,000 people. In response to low doctor/patient ratios the majority of PICs have expanded their nursing education in order to build out their health workforce.
Vulnerable health system infrastructure: This topic covered the vulnerability of the hardscaping of health systems in PICs, the buildings, to extreme weather events and rising sea levels. Two talks on this topic generated long robust discussions about health infrastructure including hospitals, clinics, dispensaries and their accessibility during extreme weather events. The majority of Pacific Island Country representatives expressed deep concern about where their health facility infrastructure is built, what materials are used in the building process and where funding for adaptation renovation or relocation would come from.
The discussion that followed each topic presented was what most impressed me. Comments made by the Permanent Secretaries reflected the consistency of the types of issues faced by Pacific Island Countries across the Blue Continent. Representatives shared their experiences, frustrations and advice. One discussion following a talk on creating climate resilient health systems highlighted the difficulty some PICs have applying for climate adaptation funding. While Tuvalu has been awarded Green Climate Funds to address infrastructure adaptation both Cook Islands and Kiribati discussed the tedious nature of the application process that can take up to 5 years to be awarded.
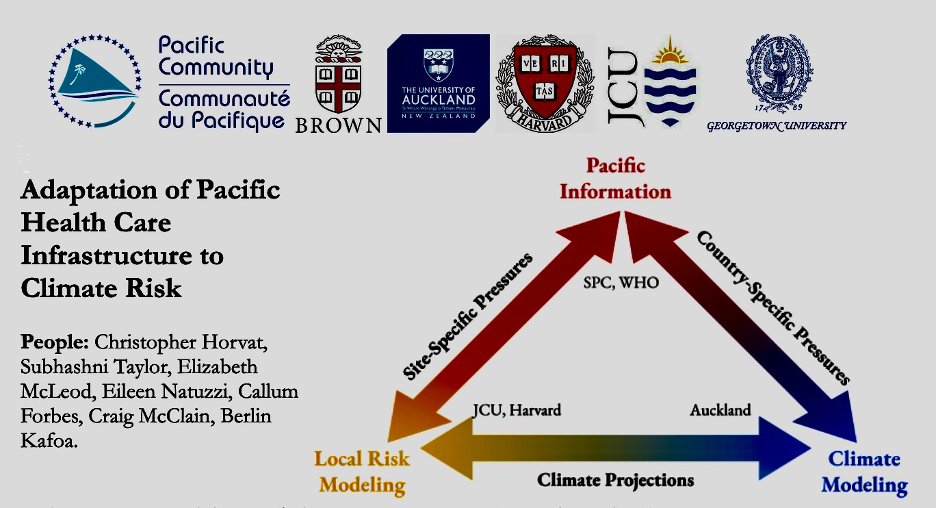 In response to climate impacts on health systems, the SPC’s Division of Public Health, headed by Berlin Kafoa and Sunia Soakai, has assembled a group of health and climate researchers tasked with producing a detailed assessment of vulnerable health facility hardscaping in the region. The assessment will include the means by which health facilities are accessed including paths, roads, bridges, ports and airstrips and the availability of basic utilities such as water, sewage and electricity. Health workforce and population census data will also be collected. This base information will have layered upon it model projections of rising sea levels, storm surge, cyclones and drought. The project starts by looking at 3 countries representing the 3 regions in the Pacific: Tonga (Polynesia), Kiribati (Micronesia) and Solomon Islands (Melanesia). Seven of us are working on this project bringing together SPC and a number of US and Australian universities. Our goal is to extend the model out to every PIC health system in order to define their vulnerability. The data generated from this work will be used by Pacific Island Country leaders to plan for and obtain funding for smart and safe health system adaptation throughout the region. SPC’s Division of Public Health is committed to obtaining quality data that can be applied across the Blue Continent where climate mediated threats such as extreme weather events and sea level rise are already “locked in.” The Adaptation of Pacific Health Care Infrastructure to Climate Risk team aims to present the initial study to the Pacific Heads of Health next year.
In response to climate impacts on health systems, the SPC’s Division of Public Health, headed by Berlin Kafoa and Sunia Soakai, has assembled a group of health and climate researchers tasked with producing a detailed assessment of vulnerable health facility hardscaping in the region. The assessment will include the means by which health facilities are accessed including paths, roads, bridges, ports and airstrips and the availability of basic utilities such as water, sewage and electricity. Health workforce and population census data will also be collected. This base information will have layered upon it model projections of rising sea levels, storm surge, cyclones and drought. The project starts by looking at 3 countries representing the 3 regions in the Pacific: Tonga (Polynesia), Kiribati (Micronesia) and Solomon Islands (Melanesia). Seven of us are working on this project bringing together SPC and a number of US and Australian universities. Our goal is to extend the model out to every PIC health system in order to define their vulnerability. The data generated from this work will be used by Pacific Island Country leaders to plan for and obtain funding for smart and safe health system adaptation throughout the region. SPC’s Division of Public Health is committed to obtaining quality data that can be applied across the Blue Continent where climate mediated threats such as extreme weather events and sea level rise are already “locked in.” The Adaptation of Pacific Health Care Infrastructure to Climate Risk team aims to present the initial study to the Pacific Heads of Health next year.
Eileen Natuzzi is an affiliate of the Center for Australian, New Zealand and Pacific Studies located in the School of Foreign Service at Georgetown University. She currently serves as Solomon Island’s co-coordinator for the Australia New Zealand Gastrointestinal International Training Association (ANZGITA) and is a visiting staff member at the National Referral Hospital (NRH) in Honiara, Guadalcanal.